WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)?
Hallux Rigidus is a common term for arthritis of the metatarsophalangeal joint of the big toe. Hallux is Latin for great toe and Rigidus is Latin meaning ‘stiff’. Hallux rigidus is a condition caused by arthritis (wear and tear) at the base of the big toe. This condition can affect all individuals, but is more likely to affect those who are active and regularly participate in sporting activities.
Patients may feel a lump on top of the big toe, whereas the prominence in hallux valgus (bunion) is seen on the medial side of the big toe. Pain is increased when walking or running. This is caused by the upward movement of the toe where joint stiffness is most evident.
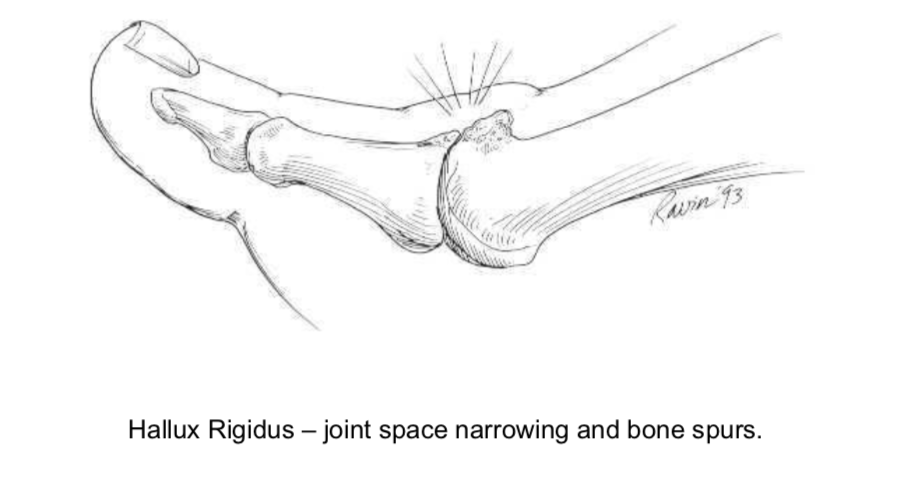
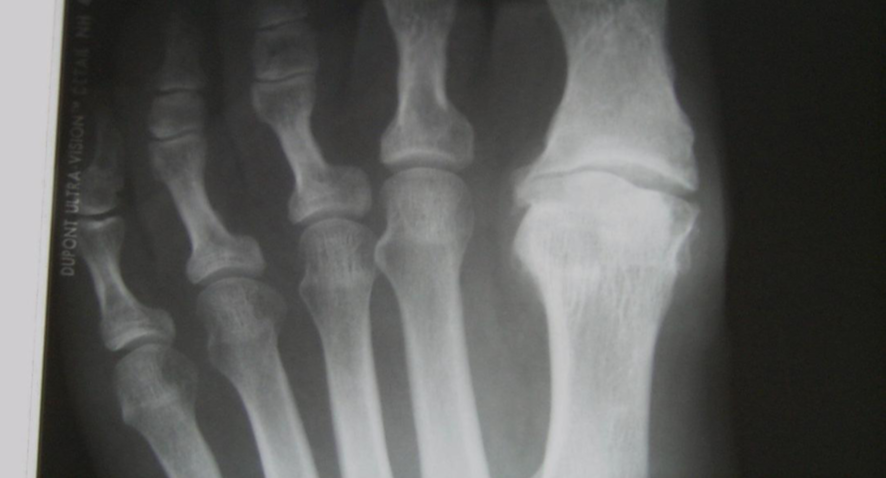
TREATMENT
Assessment – medical evaluation will determine the type of treatment that will be most appropriate for you. Osteoarthritis (wear and tear), and rheumatoid arthritis, along with infection or gout can all cause pain in the big toe and forefoot. Circulatory conditions such as diabetes and ischaemia may also be present. These conditions may have an impact on the method of treatment that your surgeon provides.
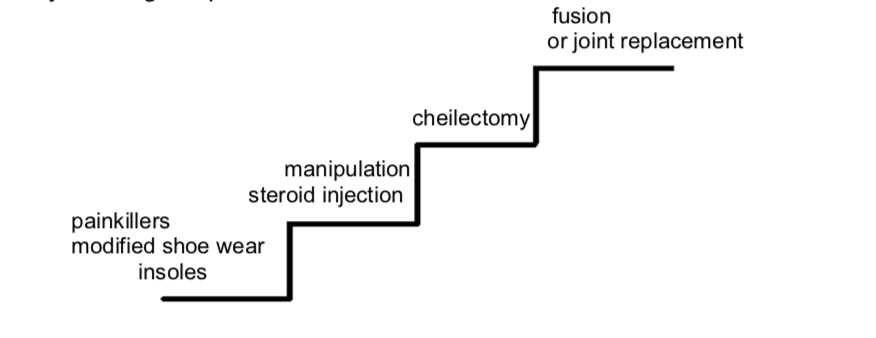
Non-surgical methods of treatment
Early or mild arthritis may be treated using non -nvasive procedures such as insoles. It is possible to manage hallux rigidus by adapting your footwear and wearing shoes with a firm sole. This may improve your symptoms. Tender areas on top of the big toe that are uncomfortable may be relieved by the use of protective pads made of silicone and other materials. These provide cushioning to prominent or tender areas.
Prescribed medications – These contain anti-inflammatory properties that may help to reduce discomfort. Anti-inflammatory gels applied topically may also be effective in the relief of symptoms.
Manipulation and steroid injection – This procedure does not involve any surgical cuts but is usually carried out under general anaesthesia as a day case procedure: a manipulation is performed to release the contracture of the joint to allow more movement and reduce pain; a steroid injection into the joint also helps to reduce pain and inflammation. You can remove the dressing after 24 hours and return to all normal activities. The joint may become more painful for a few weeks in a tiny minority of patients. Pain relief is obtained in about 50% of patients for up to 2 years but the procedure does not cure the underlying arthritis and further treatment has to be considered later. We will discuss the procedure with you as a method of delaying surgical methods of treatment if you have mild to moderate arthritis in the joint.
Surgery should only be considered if all non surgical measures have been explored OR if symptoms are significant.
Surgical methods of treatment
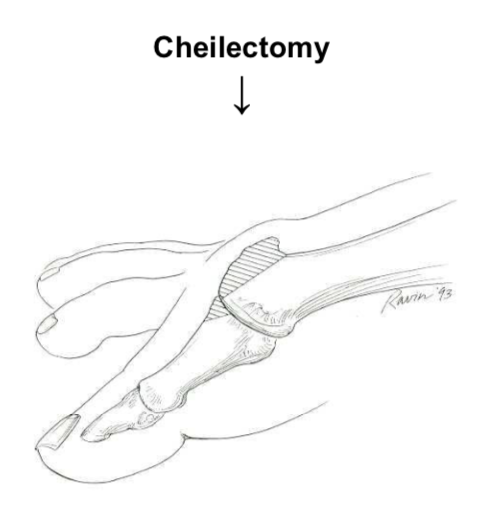
This procedure involves removing the extra bump of bone on top of the big toe that is causing pain and discomfort; it does not cure the arthritic process. By performing this operation, movement in the joint of the big toe is increased. For those patients with less severe arthritis there is an 80% chance of this surgery being successful for up to 5 years. If a cheilectomy fails to improve your condition, then a fusion may be undertaken at a later date.
Fusion
This operation is performed to correct deformity, relieve pain and improve function. The aim of the procedure is to ‘fix’ the bones in the big toe. The operation involves holding raw bone edges together until they unite (join). The joints are exposed and degenerate surfaces are cleared away and bony prominences are removed. The metatarsal bone (the bone at the base of the big toe) is fused to the phalanx (toe bone). The bone is held in position by metal such as a plate or two small surgical screws. The ‘fix’ is stable and there is usually no need for a cast post operatively. The body is ‘tricked’ into treating the joint as it would a broken bone and bone grows across the joint fusing it solid. This produces a stiff joint and the ability to bend the toe at the metatarsophalangeal joint is lost. However, you will still be able to bend the toe at the interphalangeal joint,
The X ray below indicates the joints involved in the procedure, which converts a relatively stiff painful metatarsophalangeal joint into a totally stiff painless joint.
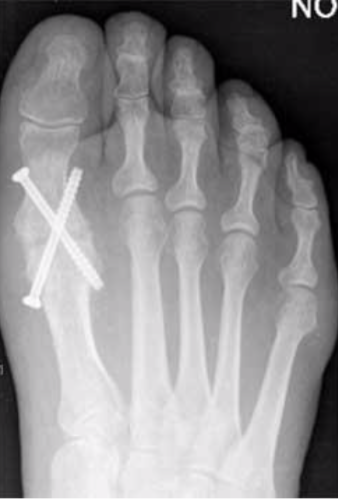
Most forefoot surgery is carried out as a day case and does not involve an over night stay in hospital. However, sometimes it is necessary to stay in hospital for one night. This will depend upon your general health and how quickly you recover from the operation. Your surgeon will advise you of the most suitable choice for you.
Anaesthesia – either a general anaesthesia (asleep) or an ankle block using local anaesthetic (awake). In both instances, a lower leg/ankle block is performed by using a local anaesthetic that is injected locally. This provides pain relief following the procedure. Your anaesthetist will discuss this and offer advice regarding the most suitable method of anaesthesia.
IMPORTANT POSTOPERATIVE ADVICE
Following your operation – when you arrive back to the ward from theatre your foot will be elevated and you will have a padded bandage on.
Wound site – you will either have stitches or steristrips in-situ with a dressing covering the wound(s). It is extremely important to keep your leg elevated to above groin level for the first 72 hours following the operation. This greatly helps to limit swelling and reduce post operative complications. It is unlikely that you will need crutches. A physiotherapist will assess and instruct you and will usually provide you with a post-op shoe. In some circumstances, a cast will be applied. Obviously, you must keep the foot clean and dry, protecting it when you have a bath or shower until the wound is fully healed.
An appointment to attend the outpatient department two weeks following your procedure will be arranged. The bandage and dressings will be removed along with any stitches and your wound site will be inspected.
Cheilectomy – the recovery period is usually quicker for this operation than for a fusion. It is important that you exercise the joint by holding your big toe and gently moving it up and down. Performing these exercises regularly and at an early stage following surgery allows the best possible result from your surgery. Swelling after this operation persists for about 3 months. As raw bone is left, you do not start feeling the benefit of the operation until about 6 weeks after the operation, and your symptoms should then continue to improve for up to 12 months.
Fusion – the recovery period for a fusion is a lengthier process than that of a cheilectomy. It will take about 6 weeks for your pain level to reduce and the pain and swelling will continue to improve for up to 12 months. You will be provided with a wedge shoe to wear following your operation. This shoe is designed to alleviate the weight from the front of your foot so the weight is taken through the rear of your foot. This shoe will be worn for 6 to 8 weeks following your surgery. It will be a further 6 to 8 weeks before you are able to wear a standard shoe.
Returning to work – this depends on the type of operation you have had. If you have a cheilectomy and have an office or sedentary type of employment with provisions for you to elevate the affected limb then you may resume work following your 2 week out patient appointment. If you have had a fusion, then it is usually 6 to 8 weeks before you can comfortably resume work. However, if your employment is physically demanding and involves long periods on your feet then it is advisable to refrain from work for a longer period of time. This decision will entirely depend on your type of employment and how you get to work etc…
Driving – if you have a fusion or cheilectomy on the left foot and an automatic car you can usually drive following your 2 week out patient appointment if all is well. You must be able to perform an emergency stop. Notify your insurance company of the type of operation that you have undergone to ensure that cover is valid.
Sport – if you have had a cheilectomy then returning to sport will be much sooner. If you have had a fusion you can usually resume sport between 3 and 6 months. Vigorous sports such as football, squash etc… is unlikely following a fusion.
POSSIBLE COMPLICATIONS OF SURGERY
Infection – this occasionally occurs in a small percentage of patients. However, if this is the case, then it is possible that further surgery may be required to remove infected bone or screws/pins. Minor infections are slightly more common and normally settle after a short course of antibiotics.
Numbness or tingling – at the surgical site(s) can occur as a result of minor nerve damage. Often this is temporary; however, the numbness or sensitised area may be permanent.
Incision site – The outer surface of the foot where the blood supply is not so good may be slow to heal. If this is the case, more frequent wound dressings may be required to ensure that the wound does not become infected.
Failure to relieve pain – patients may continue to have pain and or stiffness following cheilectomy; they may then require a fusion. Very occasionally, patients with a fusion may continue to have pain also.
Position – (fusion patients only), research has shown that 5-10 % of fusions do not heal in the exact position intended. This may be either due to the fact that the position was not achieved at the time of surgery, or that the bones have shifted. Women will find that they cannot wear high heels after a fusion.
Non union (fusion surgery only) – occasionally bones fail to unite (not join). If you smoke your risk of non union or major complications are greatly increased. It is therefore essential that you stop smoking before surgery and refrain from smoking until all bones have healed.
Screws – occasionally they may need to be removed if prominent.
Scarring – any type of surgery will leave a scar. Occasionally this causes pain and irritation.
Blood clots – Deep vein thrombosis (D.V.T.) or Pulmonary Embolus (P.E.) are rare. Please inform the team if you have had a D.V.T. or P.E. before or if you have a family history of clotting disorders.
This article is intended to inform and give insight but not treat, diagnose or replace the advice of a doctor. Always seek medical advice with any questions regarding a medical condition.

